Here at Vein Health Clinics, we’re dedicated to caring for your overall health, which includes helping you with restless legs syndrome (RLS).
Although we frequently screen for RLS because it’s a warning sign of peripheral vascular disease, we also participate in National Restless Legs Awareness Day on September 23rd, raising your awareness with in-depth information about RLS.
Restless legs syndrome symptoms
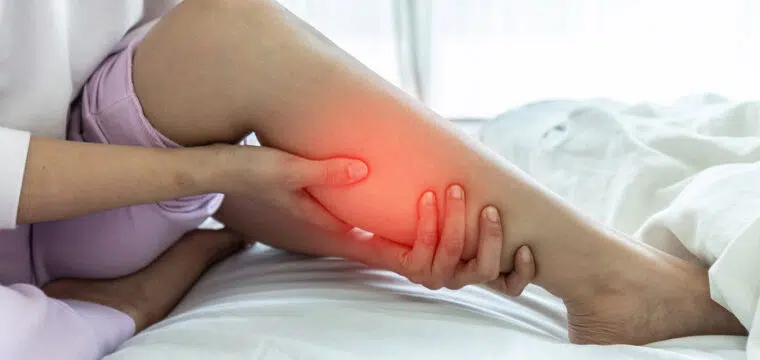
RLS occurs when you sit for a long time, like in the movie theater, or when you lie down to sleep. As soon as you relax, you get an uncontrollable urge to move your legs.
The key characteristics of RLS are:
- Symptoms begin when you rest and worsen at night
- Leg twitching and kicking occur throughout the night
- Unpleasant sensations occur, such as crawling, creeping, or itching
- Symptoms improve if you get up and move or stretch
You also won’t be able to get a good night’s sleep, so you struggle to have energy during the day.
Causes of restless legs syndrome
In some cases, RLS is inherited, so you’ll have a higher risk of developing the condition if it runs in your family.
Although the experts are still studying RLS to tie down its exact cause, research so far shows several possible sources:
Imbalanced brain chemicals
RLS is associated with dysfunction in areas of the brain that control movement. These areas are activated by a neurotransmitter called dopamine, which is essential for producing purposeful and smooth muscle movements. Any problem affecting dopamine levels can lead to involuntary muscle movements, such as those that occur in RLS.
Iron deficiency
A shortage of iron in your brain or a problem in the way your brain uses iron can cause RLS, possibly because iron is needed to produce dopamine.
Brain levels of iron may drop due to an iron deficiency. You can develop an iron deficiency if you don’t get enough iron in your diet, or if you have problems absorbing the iron you consume.
Iron deficiency also occurs when you lose more iron through bleeding than your body can replace through normal iron production. This type of bleeding arises from slow but ongoing bleeding due to gastrointestinal disease and in women with heavy menstrual periods.
Underlying health conditions
Your risk of developing RLS increases when you have an underlying health condition such as:
- Kidney disease
- Parkinson’s disease
- Diabetes
- Rheumatoid arthritis
- Sjogren’s syndrome
Some of these conditions may cause RLS by affecting the amount of iron in your brain. For example, kidney disease, diabetes, and medications used to treat diabetes can lead to iron deficiency.
Pregnancy
Up to a third of women develop RLS during pregnancy, possibly due to a family history of RLS, low iron, hormones, vitamin D deficiency, or any combination of these factors.
RLS goes away in the weeks after delivery for most women, but for others, it may linger for years. Your risk of developing RLS in the future is four times higher than the average risk if you have RLS while you’re pregnant.
Medications
Several types of medications are known to trigger RLS, such as:
- Anti-nausea medications
- Antidepressants
- Antipsychotics
- Antihistamines
- Calcium channel blockers
If a medication is the primary cause of RLS, your symptoms should go away when your doctor prescribes a different drug.
Treatment options for restless legs syndrome
Treatment for RLS is determined by the severity of your symptoms and may include:
Iron supplements
If blood tests show you have an iron deficiency, then iron supplements are the first line of treatment. If supplements don’t boost your iron, you may need an intravenous infusion to restore iron and relieve RLS symptoms.
Medication
You may benefit from one of several medications that increase dopamine levels and are approved by the US Food and Drug Administration to treat moderate-to-severe RLS. Other medication options include muscle relaxants and anti-seizure medications that help prevent unpleasant sensations.
Medical devices
One type of medical device wraps around your feet. By applying pressure to foot muscles, the wrap delivers an acupressure effect that relieves symptoms. It may also stimulate the release of dopamine in your brain.
In clinical trials, the foot wrap significantly improved symptoms and made it possible for patients to get more sleep.
Another medical device, called Relaxis®, is a vibrating pad that gently stimulates your legs. It interrupts RLS by overwhelming the unpleasant sensations, similar to the relief you’d get from walking or stretching.
If you suffer from the uncomfortable symptoms of RLS, call Vein Health Clinics for a thorough examination and customized treatment. Or you can click the “book online” button while you’re here on the website.
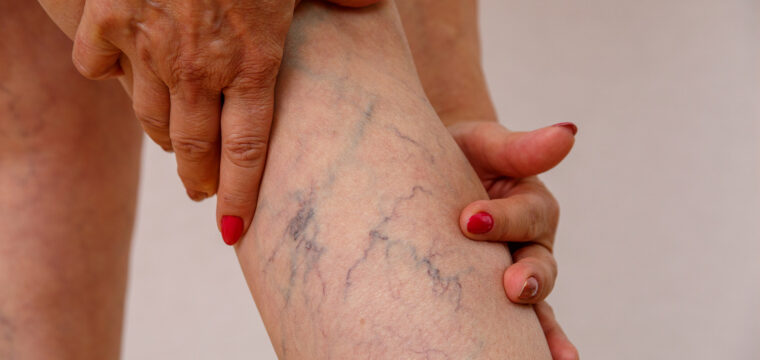
If you’re at risk of developing spider veins, you may also be more susceptible to RLS. For more information on spider veins and your risk of developing them, check out this tor blog from Vein Health Clinics: 5 Factors that Increase Your Risk of Developing Spider Veins.