Pelvic congestion affects up to 15% of all women and is responsible for about one-third of all cases of chronic pelvic pain. If you have ongoing pelvic pain, and your OB/GYN rules out gynecological problems, it’s time to look for help in an unexpected place: with the specialists at Vein Health Clinics. Your chronic pelvic pain may be due to a vein problem called pelvic congestion.
Pelvic congestion syndrome explained
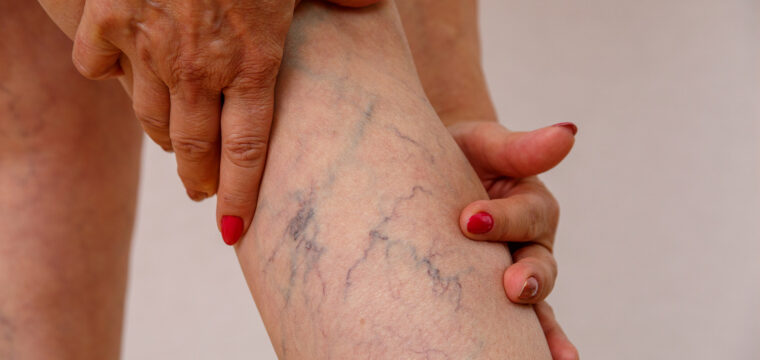
Pelvic congestion, or pelvic congestion syndrome, refers to congested veins, which are varicose veins that have become engorged with blood. In pelvic congestion, the varicosities develop in the ovarian and iliac veins that serve your pelvic region.
Causes of pelvic congestion
Two conditions contribute to pelvic congestion:
Dysfunctional valves
Pelvic congestion occurs when valves in the veins fail to work properly. The pelvic veins carry blood back to your heart, forcing blood up through the abdomen against gravity and pressure from your body.
To keep blood flowing in the right direction, veins have valves that open to let blood go up through the vein, then close to stop it from flowing backward. When a valve weakens or becomes damaged, blood goes downward and backs up. Congested veins start to bulge, twist, and cause pain.
Pelvic congestion often develops during pregnancy, when the veins widen to facilitate the increased blood flow. As the veins enlarge, the valves may be stretched or weakened, leading to backward blood flow.
Iliac vein stenosis
About 80% of women with congested ovarian veins also have a narrowing of the iliac vein. This narrowing blocks blood flow and contributes to varicosities.
Symptoms of pelvic congestion
Pelvic congestion causes one primary symptom: pain. The condition begins with general pelvic pain that may be dull or sharp. Many women find that their pain worsens throughout the day, then feel better after lying down all night.
You may also have pain during or after intercourse, and your pain may increase during your menstrual periods. In addition to pelvic pain, you may have lower back pain or an achy feeling in your legs.
Some women with pelvic congestion have abnormal vaginal bleeding or a watery discharge from the vagina. Although less common, pelvic congestion can cause progressive hip pain. You may also experience headaches and abdominal bloating.
Treatments for pelvic congestion
Medications may help relieve your pain, but their effect is short-lived and doesn’t get to the source of the problem. We provide long-term pain relief by performing the gold-standard pelvic congestion treatment: embolization. However, the first step is to confirm your diagnosis through an imaging procedure called venography.
During a venogram, we inject a contrasting dye and then use a specialized X-ray to view blood flow through the pelvic veins. This test gives us a definitive diagnosis, reveals the severity of the problem, and shows the precise location of the affected veins. After your venogram, we can proceed with one of the following treatments:
Transcatheter embolization
Embolization is an outpatient procedure in which we permanently stop blood flow through the varicose veins. Using real-time X-ray imaging, we guide a catheter through the veins until it reaches the site of varicosity.
Once the catheter is in place, we close the vein and block the blood flow using one of several possible techniques. In many cases, we inject a medication called a sclerosing agent, which collapses the vein and causes scarring that’s gradually resorbed. As a result, the varicose vein is eliminated, and normal blood flow continues through other veins. We may also insert coils or use a plug, sponge, or glue-like substance to effectively and safely embolize the veins.
Treatment with embolization is successful in 99% of patients, providing long-lasting pain relief for most women.
Iliac vein stenting
When we determine that narrowing of the iliac vein contributes to your pelvic congestion, we insert a stent, which holds the vein open to allow normal blood flow. Iliac vein stenting may be done alone or together with ovarian vein embolization.
If you suffer from chronic pelvic pain, contact Vein Health Clinics for a thorough evaluation to determine if your pain is caused by pelvic congestion. Use the “book online” button or call one of our clinics in Oviedo, Winter Haven, or Apopka, Florida.
Frequently Asked Questions
How To Relieve Pelvic Congestion Syndrome Pain?
To relieve pelvic congestion syndrome pain, you can try over-the-counter pain medications, wear compression stockings, exercise regularly, and avoid prolonged sitting or standing.
Does Pelvic Congestion Syndrome Cause Bloating?
Yes, pelvic congestion syndrome can cause bloating as a result of enlarged and swollen veins in the pelvic region.
How To Treat Pelvic Congestion Syndrome Naturally?
To treat pelvic congestion syndrome naturally, you can try lifestyle changes such as exercising regularly, wearing compression stockings, and avoiding prolonged sitting or standing. Herbal remedies and acupuncture may also provide some relief.
Can Pelvic Congestion Syndrome Cause Hip Pain?
Yes, pelvic congestion syndrome can cause hip pain as a result of the enlarged and swollen veins in the pelvic region putting pressure on the nerves in the hip area.
What Are Prominent Adnexal Vessels?
Prominent adnexal vessels refer to the appearance of enlarged and swollen veins in the pelvic region, which can be a symptom of pelvic congestion syndrome.
What Is The Treatment For Pelvic Congestion Syndrome?
The treatment for pelvic congestion syndrome may include lifestyle changes, such as exercising regularly and wearing compression stockings, as well as medical treatments such as embolization or surgery.
Does Pelvic Congestion Syndrome Cause Weight Gain?
Pelvic congestion syndrome can cause weight gain due to the enlarged and swollen veins in the pelvic region, which can put pressure on the digestive organs and cause bloating.
Is Pelvic Congestion Syndrome A Disability?
Pelvic congestion syndrome is not generally considered a disability, but it can cause chronic pain and discomfort that may impact daily activities and quality of life. Treatment can help manage symptoms and improve quality of life.