Many women suffer significant and often debilitating pelvic pain that may be due to pelvic congestion syndrome, a condition caused by varicose veins deep within their pelvic region. Because there are so many potential reasons for pelvic pain, this condition often goes undiagnosed and remains essentially untreated. The pain you feel with pelvic congestion is often very similar to what you might experience with issues affecting your urinary system, digestive system, or reproductive organs. Ovarian cysts, endometriosis, uterine fibroids, bladder inflammation (cystitis), and numerous other medical conditions often cause the same dull, throbbing, or sharp pain that’s also associated with pelvic congestion. And some women who have varicose veins in their pelvic region don’t have significant symptoms.
With such a wide variety of possibilities, it often takes extensive investigation to discover the underlying cause of your pelvic discomfort. As a well-respected vein specialist, Dr. Nwobi is very familiar with the subtle difference in symptoms that are related to pelvic congestion syndrome versus other issues. He’s happy to provide some insight about chronic pelvic pain that’s due to varicose veins.
What is pelvic congestion syndrome?
It takes a simplified look at the circulatory system to better understand pelvic congestion syndrome. Your body uses arteries that start at your heart to transport oxygen and other vital nutrients to your organs, including your ovaries and other structures in your pelvis. Your veins then carry the deoxygenated blood back to your heart for a refill, and the process begins again.
Normally, this continuous circulatory loop functions smoothly without your awareness. Sometimes, however, your veins can dilate or widen and may become coiled or twisted, which can cause the tiny valves in your veins that regulate blood flow to malfunction.
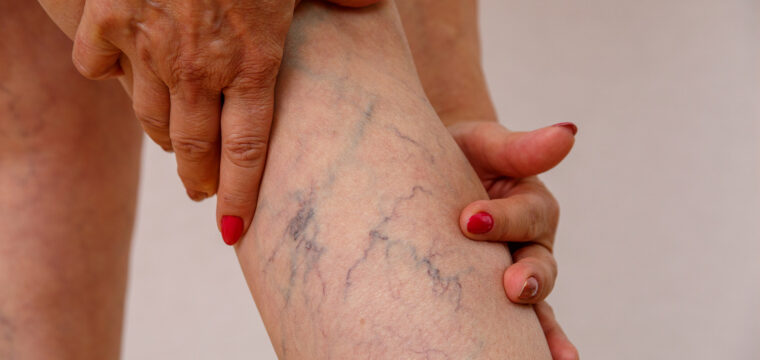
These problems create varicose veins. Pain develops when blood has difficulty moving through all the twists and turns of affected veins and it begins to accumulate.
Most people associate varicose veins with legs and feet, and it’s true that these veins are often most visible and more commonly noted in your lower extremities. You may, however, develop varicose veins deep in your pelvic region that can become quite painful, which is the underlying cause of pelvic congestion syndrome.
What are the symptoms of pelvic congestion syndrome?
Pelvic congestion can cause a dull ache throughout your lower abdomen or a sharp, throbbing pain that’s more localized to a certain area. Many conditions can cause similar pain, but other symptoms may point to the possibility of pelvic congestion. For instance, your pain may:
- Develop after you have your first child and worsen with every pregnancy
- Be worse at the end of the day
- Decrease when you lie down
- Increase with certain changes in posture, such as bending over from a sitting position
- Occur or worsen after certain physical activities, such as cycling or horseback riding
Other symptoms of pelvic congestion syndrome may include:
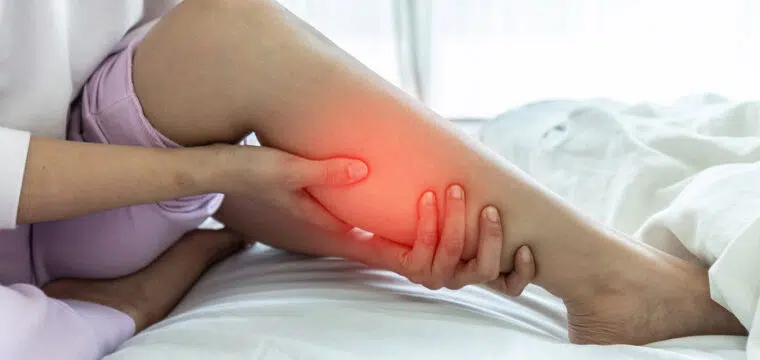
- Aching in the legs
- Lower back pain
- Abnormal vaginal bleeding
- Clear or watery vaginal discharge
- Abdominal bloating
Many women also report mood swings, headaches, and fatigue, which may be a consequence of the emotional and physical stress that occurs when you’re forced to live with chronic pain. And distress may worsen when physicians can’t seem to pinpoint a reason for your pain.
How is pelvic congestion diagnosed and treated?
Depending on other diagnostic studies you’ve already undergone, we may suggest:
- Urine studies to check for urinary system problems and others that may cause pelvic pain
- Blood tests to rule out pregnancy, anemia, and other issues
- Ultrasound to check for abnormal growths in the pelvis
If you’ve already had a thorough workup for your pelvic pain without a cause identified, and if pelvic congestion is suspected, we may recommend:
- A Doppler ultrasound to check the flow in your pelvic blood vessels
- Specialized X-rays of your pelvic veins (venography), during which we instill dye into the veins and monitor the blood flow
Treatment varies according to the severity of your symptoms but is often similar to procedures performed for other varicose veins. It may include nonsurgical remedies such as sclerotherapy or embolization to intentionally plug or seal off the varicose veins. These procedures are typically outpatient and don’t require an overnight hospital stay.
If you’ve been experiencing pelvic pain and have been unsuccessful in determining the cause, contact Vein Health Clinics today to book a consultation.
Frequently Asked Questions
Can Pelvic Congestion Syndrome Cause Dizzy Spells?
Yes, Pelvic Congestion Syndrome can cause dizzy spells due to the pressure it causes on blood vessels in the pelvic area, leading to reduced blood flow and oxygen to the brain. This can cause dizziness, lightheadedness, and other symptoms like chronic pelvic pain and varicose veins in the pelvic area.
Is Pelvic Congestion Syndrome Serious?
Pelvic Congestion Syndrome (PCS) is not life-threatening but can significantly impact a person’s quality of life. PCS can cause chronic pelvic pain, discomfort during sex, and other symptoms. Treatment options like medication, surgery, or minimally invasive procedures are available to manage symptoms and improve a person’s quality of life.
Can Pelvic Congestion Syndrome Cause Heart Problems?
No direct link exists between Pelvic Congestion Syndrome (PCS) and heart problems. However, the decreased blood flow and oxygen to the heart due to pressure on blood vessels in the pelvic area can lead to symptoms like chest pain or shortness of breath.
Can Pelvic Congestion Syndrome Cause Leg Pain?
Yes, Pelvic Congestion Syndrome (PCS) can cause leg pain. The increased pressure on blood vessels in the pelvic area can cause varicose veins, leading to leg pain, heaviness, swelling, and discomfort. Treatment options like medication, surgery, or minimally invasive procedures are available to manage PCS symptoms and relieve leg pain.
Can You Die From Pelvic Congestion Syndrome?
Pelvic Congestion Syndrome (PCS) is not life-threatening, and PCS causes no reported deaths. However, it can significantly impact a person’s quality of life, causing chronic pelvic pain, discomfort during sex, and other symptoms. Treatment options are available to manage symptoms and improve quality of life.
Does Pelvic Congestion Syndrome Cause Weight Gain?
Pelvic Congestion Syndrome (PCS) is not directly linked to weight gain. However, chronic pelvic pain and discomfort caused by PCS can lead to decreased physical activity and a sedentary lifestyle, potentially contributing to weight gain.